Long-term care hospitals need to make long-term improvements
Caregivers at the Hyo Plus hospital for the elderly in Bucheon, Gyeonggi, recall with a shudder last December, the month that the hospital became a hot spot of Covid-19 infections.“It was like hell broke loose,” one caregiver told the JoongAng Ilbo.
The hospital saw the beginning of its cluster of infections when six staff members tested positive on Dec. 11, 2020. By Jan. 3, 2021, the cases had grown to 160 total, including patients and staff members, of whom 47 died.
During this time, all but one of the hospital's 22 caregivers were infected.
The remaining doctors and nurses had to fill their shoes and carry out roles such as changing the diapers of the patients, helping them eat and brushing their teeth.
Some realized for the first time that the caregivers were asked to do too many things at once.
Nursing homes and long-term care hospitals throughout the world came under the spotlight last year for giving way to surges of Covid-19 infections and resulting in alarming rates of death. In Korea, nearly a quarter of coronavirus-related deaths in 2020 concerned elderly patients who were infected at long-term care hospitals, according to Korea Disease Control and Prevention Agency, Korea’s authority on Covid-19 response.
Part of the reason, according to some caregivers, may have to do with how understaffed the long-term care hospitals were.
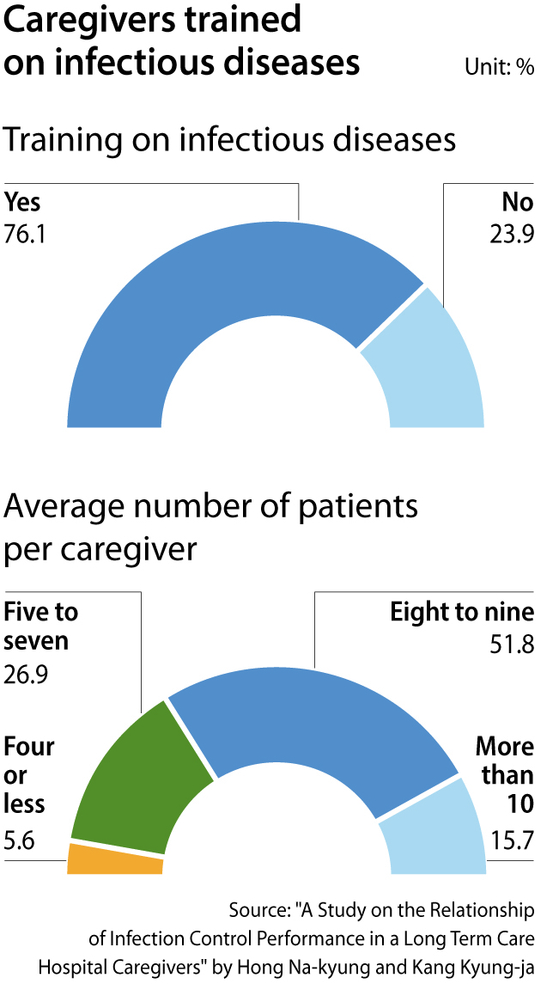
According to a survey on 197 caregivers at eight long-term care hospitals in Korea by Hong Na-kyung, a nurse at Jeju Medical Center and Kang Kyung-ja, a professor of nursing at Jeju National University, in January 2020, one caregiver takes care of an average of 7.9 patients at these hospitals.
Another study by Myoung Soon-koo, a professor of law at Korea University, and his team in 2018 found that some caregivers are asked to take care of over ten, even 20 patients at a time.
For the sake of efficiency, some nursing homes and hospitals, including Hyo Plus hospital, put as many as 24 patients into one ward.
According to Health Insurance Review and Assessment Service, out of 250,000 wards at long-term care hospitals in Korea, 8 percent, or 19,696 wards, are for 10 or more people. Of these, nearly half of them are for 14 or more.
These wards were especially problematic during the pandemic. In addition to Hyo Plus hospital, other hospitals that had large-sized wards quickly became Covid-19 hot spots.
Miso Hospital, a long-term care hospital in Goyang, Gyeonggi, has a 20-person ward. All of the patients and caregivers of the ward were infected with Covid-19 last year.
None of these long-term care hospitals were required by law to train the medical staff members on how to prevent the spread of infectious diseases.
“I’ve been working across long-term care hospitals for the past seven years and I didn’t see much training on prevention of infectious diseases,” a 60-year-old caregiver told the JoongAng Ilbo.
Every hospital in Korea needs a government inspection every three years and needs to meet some minimum requirements to continue operating as a medical institution. For general hospitals, requirements include training of staff members on prevention of infectious diseases.
Long-term care hospitals for the elderly, however, are an exception to the rule. There is no state budget set aside for training at the long-term care hospitals, unlike general hospitals.
“It’s an anomaly, because nursing homes and long-term care hospitals ought to be the ones prioritized for training on infectious diseases, as these are the places where we have patients much more vulnerable to infectious diseases,” said Lee Sang-il, professor of disease prevention at University of Ulsan College of Medicine. “The pandemic has finally unveiled that situation at the nursing homes to the larger public.”
Long-term care hospitals were problematic long before the pandemic hit Korea, some experts said.
“Because we were so understaffed, we would rely on extra doses of sedatives to put the patients to sleep at night,” a nurse said in an anonymous interview with Lee So-young, a nurse who interviewed several other nurses at long-term care hospitals for her doctoral thesis at Hanyang University in 2020.
The study found that long-term care hospitals prescribed up to five times the amount of sleeping pills to patients when compared to general hospitals.
“It’s because the long-term care hospitals are understaffed and cannot attend to every patient who may scream their head off all night if they’re not attended to around the clock, for reasons such as dementia and others,” said Sohn Deok-hyun, head of Korea Convalescent Hospital Association.
The lack of caregivers also gave way to inhumane treatment of patients.
“With the serious lack of caregivers at hospitals, the caregivers have no option but to resort to some inhumane methods, like tying some patients to their beds, or force-feeding some patients who refuse to eat during the designated meal time,” reads the report by Myoung Soon-koo of Korea University and his team.
A change to the caregiver system at long-term care hospitals, according to some experts, will have to come from the way they are financed.
“The long-term care hospitals are understaffed because the caregivers are paid for by the patients,” Sohn said.
Because the wage for the caregivers comes straight from the pockets of the patients, many patients prefer to share a caregiver to reduce the burden. When six to seven patients share a caregiver, each pay around 500,000 won ($450) a month for the service, the JoongAng Ilbo found in its survey across long-term care hospitals.
Additionally, compared to general hospitals, the long-term care hospitals are not required by law to hire as many staff members.
By law, a 100-ward general hospital needs a minimum of five doctors and 40 nurses to operate.
On the other hand, a long-term care hospital of the same size requires a minimum of two doctors, six nurses and 11 caregivers.
“There could be a positive change if the government would share the cost for caregivers and set aside some of the budget to pay for them, so that more can be hired at the hospitals, for each caregiver to provide a more undivided attention to each patient,” Sohn said.
It’s time that Korea renovated its elderly care policies, said Seok Jae-un, professor of social welfare at Hallym University.
“We’re one of the fastest aging societies in the world, yet we are paying almost nothing compared to what other developed countries are paying,” said Seok. “It’s time to change that. The government ought to be investing more in long-term care hospitals. The welfare of the caregivers is closely linked with that of the patients.”
BY SPECIAL REPORTING TEAM [chung.juhee@joongang.co.kr]










with the Korea JoongAng Daily
To write comments, please log in to one of the accounts.
Standards Board Policy (0/250자)