[SECOND IN A THREE-PART SERIES] Death with dignity can be stymied legally
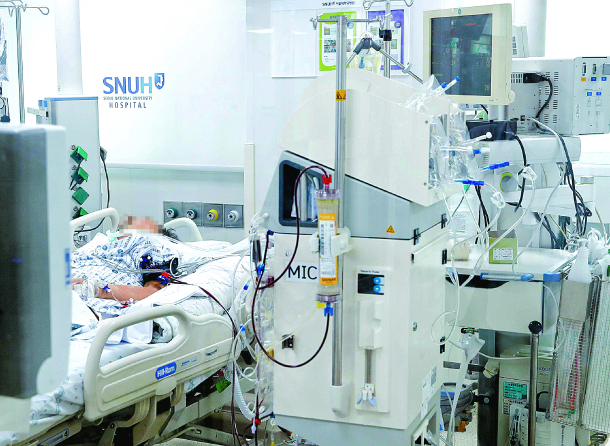
Every year, an average of 40,000 patients are left without a legal option to die with dignity because their hospitals don’t have ethics committees. The patient above is hooked up to a breathing device at an ICU in Seoul National University Hospital, which does have such a committee. [JOONGANG ILBO]
A 90-year-old woman was admitted to a hospital recently after having a very serious stroke. After she was declared brain-dead, the medical staff recommended her family sign a statement taking her off life support.
The family wanted to pull the plug and discontinue the pointless treatment - and to give the woman a dignified death. But there was a legal snag. Two of the woman’s grandchildren could not be contacted. According to the law, all legally registered family members must sign an agreement to discontinue life support for a patient.
That rigid requirement was originally intended to protect ill people from wrong decisions by their relatives, such as an impatient relative wanting to end someone’s medical treatment prematurely. Now it is an example of how legally tricky it is for a country to legally institute the concept of death with dignity.
Korea’s death with dignity law was passed in Feb. 2016 and went into effect eight months ago. It combines a do-not-resuscitate (DNR) order with an order to take a patient off life support systems.
As of now, the death with dignity law requires patients to get an official written opinion from their doctor and another doctor who specializes in the corresponding disease in order to be deemed eligible. Patients then sign an order stating that they should not receive life prolongation treatment like CPR or anticancer drugs.
In cases in which the patient is not conscious but has verbally communicated the desire not to be kept on life support systems in the past, testimonials from two family members are required to finalize the process.
Complications arise when a patient is unconscious and has never discussed the issue with relatives in the past. In that case, the death with dignity law requires that all legally registered family members sign the order ending medical treatment. The law dictates that pain relief measures and basic injections of nutrients, water and oxygen still be maintained.
“Deciding to perform CPR or use a respirator on a patient is a decision that medical staff needs to make in the immediate moment. It cannot be put on hold while the family tracks down all family members,” said Dr. Heo Dae-seog, a professor of medicine at Seoul National University who specializes in treating brain tumors at Seoul National University Hospital.
A bill revising the law to only require the signatures of the patient’s parents and/or children has been pending in the National Assembly since June. “In the case of America, patients are advised to assign a health care proxy, or surrogate - someone you trust to make health care decisions for you if you can’t speak for yourself,” said Lee Il-hak, a professor of Bioethics and Health Laws at Yonsei University. “Adopting this kind of system will help reduce confusion if the case occurs.”
Another snag that has developed is the fact that patients who have signed the order will only see it respected in hospitals that have ethics committees that can oversee the administration of the patient’s wishes.
The death with dignity law requires an ethics committee of five members, two of whom must not come from a medical background, to oversee the application process and thoroughly inform the patient and their family of the consequences to agreeing not to receive life support treatment.
But many hospitals do not have ethics committees. According to the Ministry of Health and Welfare and the Korea National Institute for Bioethics Policy, only 164 hospitals nationwide have ethics committees. There are 157 towns and cities across Korea that do not even have a medical facility with an ethics committee.
Decisions about life support often take place in ICUs (Intensive Care Units). Out of 281 hospitals with ICUs, 151 hospitals (54 percent) do not have an ethics committee. Every year, an average of 40,000 ICU patients are in medical facilities that would not allow them to die with dignity.
In the case of nursing hospitals, only 1.4 percent or 22 nursing hospitals nationwide have ethics committees. This becomes problematic when a patient who has signed an order to discontinue life support is admitted and goes into decline.
Patient Choi, who had signed such an order, was still subjected to life support treatment because the nursing hospital he was admitted to did not have access to the Korea National Institute for Bioethics Policy database that could confirm his wishes. Only ethics committees get access to the database.
“Right before the Korean War ended, medical services only required one or two signatures from the next of kin to go through with a DNR order. After the law was enacted, requirements for health treatment suspension are stricter than after the war,” said Kim So-yoon a professor of Bioethics and Health Laws at Yonsei University.
BY SPECIAL REPORTING TEAM [jeong.juwon@joongang.co.kr]










with the Korea JoongAng Daily
To write comments, please log in to one of the accounts.
Standards Board Policy (0/250자)